When Is a Tooth Extraction Necessary?
We all want to feel good about our smiles. Smiling brings happiness and makes people feel better. But sometimes, our teeth can tell a different
We are glad you have chosen us for your health needs and hope that every encounter with our offices and staff exceeds your expectations
Complete health may be our long-term goal, but our immediate priority is the patient comfort. We do our best to facilitate a relaxing office environment you’ll want to return to again and again. This includes the implementation of multiple techniques to prevent treatment discomfort and minimize anxiety.
Serving Hallandale Beach and surrounding areas since 1979, the team offers a full scope of care for the entire family.
The goal of the doctors and dentists at Delray Medical & Dental is to provide the best care to our patients in Florida.
Take advantage of the exceptional facilities and superior medical and dental care available at Coral Springs Medical & Dental.
“We tailor our programs after the six dimensions of wellness, which are physical, social, intellectual, spiritual, emotional and occupational. My role is to put on as many programs to help seniors deal mentally, emotionally, spiritually and physically with aging and chronic disease.” – Dr. James Cassidy, Director of Senior Activities
We know our patients have a choice in several different areas, so we go out of our way to deliver the level of care and compassion we would want for our own families.
Medical cannabis is a treatment option available in the state of Florida for chronic health conditions, like epilepsy and Crohn’s disease. The medical team at Hallandale Medical Center in Hallandale Beach, Florida, is authorized to prescribe medical cannabis and provide the initial health evaluation you need to qualify as a medical cannabis user with the state. You can receive a comprehensive medical evaluation to determine if you’re a good candidate for treatment with medical cannabis by calling Hallandale Medical Center today or by scheduling a consultation online now.

We all want to feel good about our smiles. Smiling brings happiness and makes people feel better. But sometimes, our teeth can tell a different
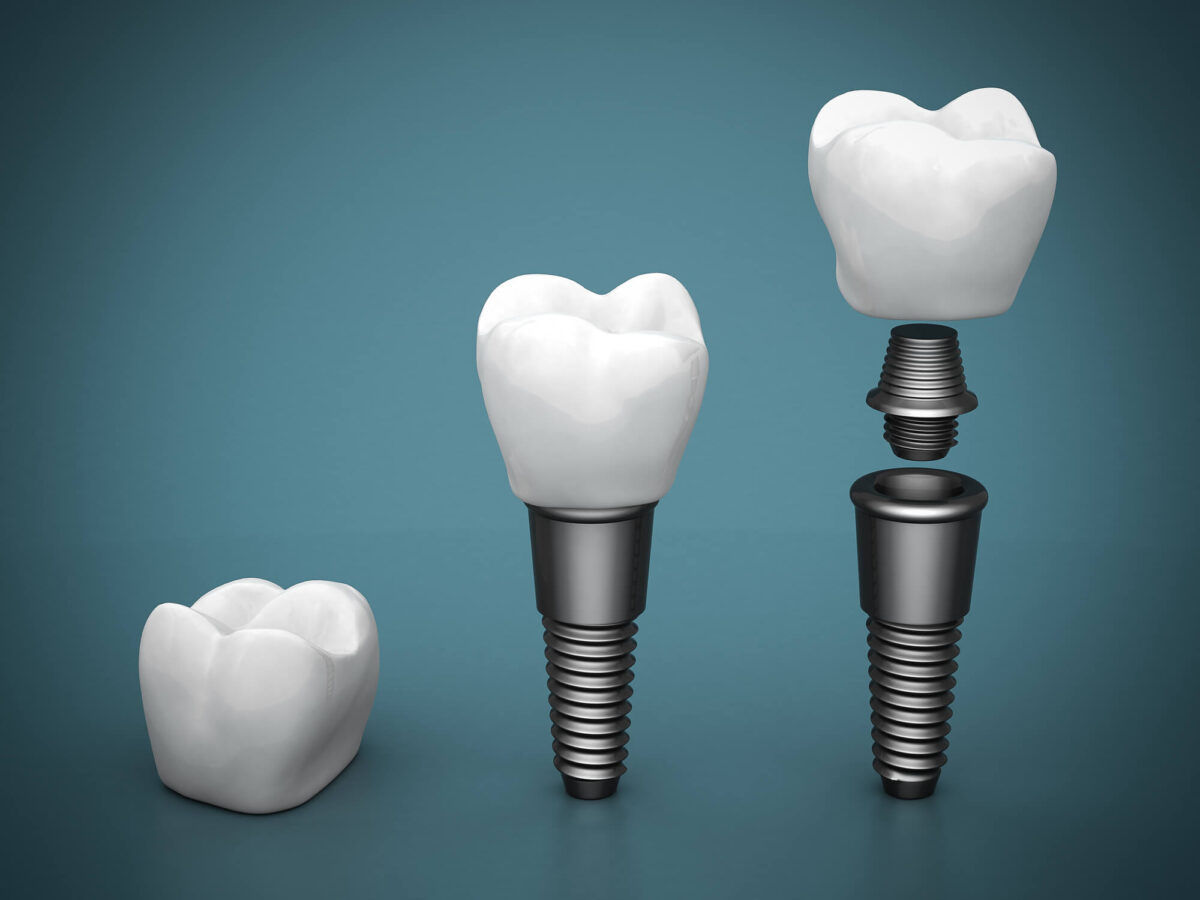
Dental implants are artificial substitutes for missing teeth. They’re metal posts surgically implanted into the jaw to support a tooth’s replacement. But like any implant,

Same-day dental in Coral Springs provides oral care that allows patients to obtain their services in a single visit. Unlike traditional dentistry, which requires patients

Our team consists of dedicated individuals who are kind, friendly, and caring. Our staff is here to ensure a pleasant experience during your visit to our office.
Our team includes experienced and energetic people whose goal is to communicate well with our patients and provide the best care possible.
If you are in search of a professional who will attend to your needs, you can’t go wrong with our practice. Contact our office at your earliest convenience to schedule your consultation. We look forward to serving you and your family for many years to come.
Our staff is key to our success. Our business model is patient-centric with an emphasis on exceptional medical care, strong provider/patient relationships, and high physician and staff to patient ratios, which allows us to dedicate the time needed to each-and-every patient and their family.








